Who Owns the Limb? Ethical Boundaries of Insurance Control Over Medical Decisions
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Cath Lab Digest or HMP Global, their employees, and affiliates.
Anamika Fnu, MD; Sakshi Dixit, MD; Anmol Multani, MD; Akiva Rosenzveig, MD; Aravinda Nanjundappa, MD
Cleveland Clinic, Cleveland, Ohio
The authors can be contacted via Akiva Rosenzveig, MD, at rosenza@ccf.org.
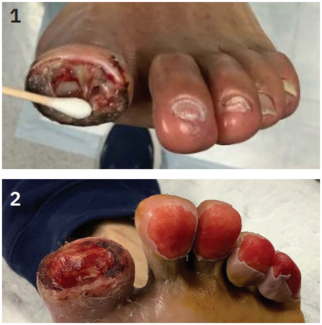
Peripheral artery disease (PAD) is a chronic atherosclerotic occlusive disorder of the lower extremity arteries and affects more than 200 million individuals worldwide.1 Chronic limb-threatening ischemia (CLTI) represents the end stage of peripheral artery disease and is characterized by ischemic rest pain and/or tissue loss.2 If left untreated, CLTI is associated with an estimated 25% risk of limb loss within one year.3 All patients with suspected or confirmed CLTI should receive optimal medical therapy and be urgently referred to a vascular specialist.3 Lower-extremity arterial revascularization is essential to prevent major above-ankle amputation in patients with CLTI and is achieved through two primary approaches: endovascular therapy and open surgical bypass.4 The 2019 Global Vascular Guidelines recommend patient-centered infrainguinal revascularization for CLTI using the PLAN framework (Patient risk, Limb stage, Anatomic pattern).3 The BEST-CLI trial demonstrated that in CLTI patients with an adequate great saphenous vein for surgical revascularization, the incidence of major adverse limb events or death was significantly lower in the surgical group compared with the endovascular group.5 Despite evidence from clinical trials and guidelines supporting revascularization, insurance denials can result in adverse patient outcomes.
Insurance plays a huge part in the prognosis of PAD patients, including the risk of amputation. Previous studies have shown that interruption of insurance coverage in PAD patients with existing commercial health insurance is associated with an increased risk of lower-extremity amputation.6 Lower median household income, Medicaid coverage, and lack of insurance are linked to a higher risk of amputation and a lower likelihood of receiving limb-salvage revascularization.6 Denial of insurance coverage for a patient’s angiogram or revascularization can worsen outcomes. Non-evidence-based and ambiguous insurance policies can delay access to critical, limb-saving interventions.
Although insurance policies aim to follow guidelines, failure to incorporate recent guideline updates, new clinical evidence, and comprehensive patient-centered evaluations can harm patient health. Each patient’s presentation is unique, and treatment decisions must be individualized, rather than strictly guided by aggregated study results. Multidisciplinary evaluation and individualized clinical judgment should be prioritized over blanket coverage decisions. When a patient’s symptoms fail to improve with conservative management, this is a clear clinical indicator that must be taken seriously by insurance providers. Decisions made solely from chart reviews or remote assessments cannot capture the full clinical context, including patient-specific factors, comorbidities, and urgency. Every week of delay in CLTI risks a limb, yet insurance policies treat it like routine care, not an emergency. Despite the fact that authorization rests with the insurance company, physicians can provide peer-to-peer advocacy or detailed clinical justifications for imaging or revascularization procedures to minimize delays or prevent denials. Comprehensive documentation is critical, serving both as a detailed account of the patient’s condition and as an advocacy tool to prevent unnecessary delays or denials of care.
Amputation, being permanent, has profound physical and emotional consequences, and should never be approached lightly. Beyond the physical consequences, amputation causes profound emotional distress and can compromise a patient’s sense of dignity and independence. Beyond limb salvage, patient-reported outcomes, including pain, mobility, and quality of life, are adversely affected by delays.
Insurance challenges affect not only patients but also physicians, who face increased administrative burdens, including repeated authorizations and documentation requirements, consuming valuable clinical time, reducing patient-facing care, and contributing to burnout among vascular specialists. Over time, this strain can diminish clinical efficiency, impair decision-making, and even affect the quality of patient care. These obstacles may erode patient-physician trust and create tension or frustration during office visits. Studies have shown that administrative tasks occupy approximately one-sixth of U.S. physicians’ working hours and significantly reduce career satisfaction.8 It also affects the U.S. healthcare system and economy by creating inefficiencies and increasing costs.
Every patient deserves access to interventions that maximize limb salvage and minimize disability. Delays in authorization for revascularization in CLTI are more than bureaucratic hurdles — they are preventable contributors to limb loss. Clinicians, not insurers, should guide procedure planning, selecting tools based on patient need and expertise. Aligning insurance processes with contemporary evidence and patient-centered care is essential to protect patients’ limbs, health, and dignity.
References
- Berchiolli R, Bertagna G, Adami D, et al. Chronic limb-threatening ischemia and the need for revascularization. J Clin Med. 2023 Apr 4; 12(7): 2682. doi:10.3390/jcm12072682
- Houghton JSM, Saratzis AN, Sayers RD, Haunton VJ. New horizons in peripheral artery disease. Age Ageing. 2024 Jun 1; 53(6): afae114. doi:10.1093/ageing/afae114
- Conte MS, Bradbury AW, Kolh P, et al; GVG Writing Group. Global vascular guidelines on the management of chronic limb-threatening ischemia. J Vasc Surg. 2019 Jun;69(6S):3S-125S.e40. doi:10.1016/j.jvs.2019.02.016
- Kinlay S. Revascularization for chronic limb-threatening ischemia-synthesizing inconsistency. J Soc Cardiovasc Angiogr Interv. 2025 Apr 1; 4(5): 102623. doi:10.1016/j.jscai.2025.102623
- Farber A, Menard MT, Conte MS, et al; BEST-CLI Investigators. Surgery or endovascular therapy for chronic limb-threatening ischemia. N Engl J Med. 2022 Dec 22; 387(25): 2305-2316. doi:10.1056/NEJMoa2207899
- Howell C, Lane A, Weinkauf C, et al. Interruption of insurance coverage and the risk of amputation in patients with pre-existing commercial health insurance and peripheral artery disease. Ann Vasc Surg. 2023 Oct; 96: 284-291. doi:10.1016/j.avsg.2023.03.015
- Hughes K, Mota L, Nunez M, et al. The effect of income and insurance on the likelihood of major leg amputation. J Vasc Surg. 2019 Aug; 70(2): 580-587. doi:10.1016/j.jvs.2018.11.028
- Woolhandler S, Himmelstein DU. Administrative work consumes one-sixth of U.S. physicians’ working hours and lowers their career satisfaction. Int J Health Serv. 2014; 44(4): 635-642. doi:10.2190/HS.44.4.a