Defining and Treating Locally Advanced Basal Cell Carcinoma
Clinical Summary
ocally Advanced Basal Cell Carcinoma (BCC): Defining Unresectability and Systemic Therapy Sequencing
-
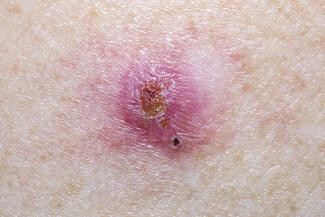
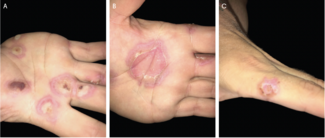
Locally advanced BCC (laBCC): Defined by inability to achieve acceptable functional/cosmetic outcomes with surgery, not size alone; features include deep invasion (beyond subcutis, bone), perineural symptoms, recurrence, or involvement of critical sites (orbit, nose, ear).
-
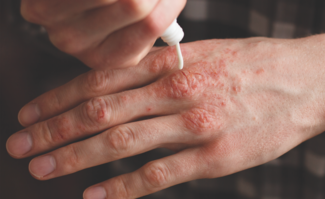
Treatment algorithm (2026): Hedgehog pathway inhibitors (vismodegib, sonidegib) remain first-line systemic therapy (≈40–60% response rates); cemiplimab (PD-1 inhibitor) is second-line for intolerance/progression, with emerging data exploring earlier immunotherapy use.
-
Patient selection: Choose therapy based on comorbidities and tolerability—hedgehog inhibitors effective but limited by chronic toxicities (dysgeusia, muscle cramps, weight loss); immunotherapy favored in frail patients or those unable to tolerate hedgehog inhibitors; multidisciplinary care essential.
Reviewed by Riya Gandhi, MA, Associate Editor of Immunology Group
Dr Vishal Patel discusses how to define locally advanced basal cell carcinoma (BCC) in real-world practice and when surgery is no longer the best option. Learn how treatment strategies have evolved with hedgehog pathway inhibitors and immunotherapy, and how patient factors, tumor characteristics, and multidisciplinary care guide optimal therapy selection.
Transcript
Hi, my name is Vishal Patel. I'm a Mohs surgeon and cutaneous oncologist based in Washington, DC at the Georgia Washington University School of Medicine, where I practice Mohs surgery and serve as the director of dermatologic surgery, as well as the director of cutaneous oncology in the GW Cancer Center.
In real-world practice, how do you define “locally advanced” BCC, and what features signal that surgery is no longer the best option?
Dr Patel: One of the challenges with basal cell carcinoma is defining locally advanced is not quite clear. There's a lot of variability there. There's not a hard and fast rule that's either defined by general staging criteria in oncology. And so definitions can differ from provider to provider, from specialty to specialty. It's less about a strict size cutoff and more whether a tumor can be treated surgically with acceptable functional and cosmetic outcomes. Sometimes I like to say rather than is something locally advanced is something easy to treat or is something going to be very difficult to treat? And that sometimes is a more clinically helpful definition in terms of advanced nature of basal cell carcinoma. We know that the vast majority are on the easy to treat side, those that are easily treated with surgical approaches, non-surgical approaches, whether that's excision mohs surgery or injections, topical therapies, photodynamic therapy, a variety of treatment options are suitable for the easy ones. But very small subset, they do become aggressive or have been delayed in treatment and then just are large and challenging to treat. And that's where we denote those as locally advanced further within the life span or the lifecycle of the disease. Now, typically, because of the nature of the presentation, these tumors have grown to be large and they begin to invade deeply into the surrounding tissue, sometimes into anatomically critical areas like the eye, the orbit, the nose, the ears, the scalp. And so other challenging features come in, in terms of how the reconstruction is going to be done, which sometimes is a defining moment more so about that repercussion of surgery than the actual presentation of the tumor itself.
Now, other features that can raise concern about more advanced or more aggressive natures, whether there's pain and symptoms and somewhere suspicious for perineural invasion, if there's invasion beyond the subcutaneous fat bone involvement, or they've been treated multiple times and it's recurred. And so ultimately, we're trying to decide whether something can technically be removed. Is surgery actually possible given that kind of complex anatomic locations we usually deal with, or if they will require extreme reconstruction, then lead to a major functional deficit, example, a loss of an eye or a significant facial impairment, impairment of speech, eating, swallowing, or something like that. And that's when we begin to think about other different management approaches.
Instead of proceeding to surgery, we may consider systemic therapies, first with hedgehog pathway inhibitors and then now we have immunotherapies as well. And so a multidisciplinary discussion is really key to understand, is surgery alone an option? Is it no longer an option? Do we need to consider a systemic therapy or do we want to start with a systemic therapy and then switch potentially to another surgical or destructive or radiation treatment option? And that's a moving target. And oftentimes with basal cell carcinoma, we don't know what we're doing from the outright, and sometimes it may be a see-and-go and go-and-see type of approach.
How has the treatment algorithm evolved, and where does immunotherapy fit relative to hedgehog inhibitors today?
Dr Patel: Yeah. There's been a significant evolution of our treatment approach or treatment algorithm for advanced basal cell carcinoma, especially in the past decade. And if you think about 10 plus years ago, we really had surgical treatment and didn't have many other non-surgical or systemic options. Once those tumors became unresectable or denoted to be unresectable and metastatic, we had limited options. And surgery and radiation were the primary modality. We would utilize that over and over again until it just no longer was an option. And that initially changed with the development of hedgehog pathway inhibitors. And at that time point, that was seen as the salvage therapy. Vismodegib, sonidegib, these are drugs that target the hedgehog pathway signaling pathway. It's that, as we know, central role in most of the development basal cell carcinomas due to mutations in the PTCH1 and smoothened gene. And these were the first systemic therapies to have meaningful activity in locally advanced metastatic disease. And as a result, based on the pivotal trials, which showed 40, 60% response rates as well as durable disease control, we would save these systemic therapies for when we exhausted surgery and radiation.
As we've moved forward, and now with the advent of immunotherapy becoming approved, that has emerged as another systemic therapeutic option, particularly it's utilized when those hedgehog pathway inhibitors are no longer working or patients cannot tolerate utilizing those medications. And so in particular, cemiplimab, a PD-1 inhibitor, was approved as a second-line indication or in patients who cannot take a hedgehog pathway inhibitor. And that opened the door a little bit in terms of being able to use hedgehog pathways earlier. It may helped us rethink about how and when we may consider systemic therapy. And so rather than only looking at surgery and radiation upfront, we may start to ask the question of hedgehog pathway inhibitors may be more appropriate upfront, maybe in a scenario, off-label type of scenario of shrinking the tumor in pseudo-neoadjuvant fashion, or maybe to try to see the response and see if patients can tolerate it and then decide whether they should switch to another surgical or non-surgical treatment.
We've learned a lot about those side effects over the last decade, and we know those hedgehog pathway inhibitors have characteristics, a risk set of side effects, taste changes, muscle cramps, alopecia, fatigue, weight loss, but they impact ... We've learned also that the drugs behave differently. And so we can modify the dosing to be able to get the most out of them. And then if patients cannot tolerate them or whether they're having progression of diseases, we can switch to immunotherapy. And there has been demonstrated responses, not nearly as what we see in squamous cell carcinoma, but certainly at a rate that we feel comfortable pivoting to that if necessary. And so generally, what we owed done 10, 15 years ago is surgery and radiation until no longer tolerable and then moving the hedgehog pathway inhibitors. Now, the treatment paradigm is does surgery make sense for the patient, but if not, we can start hedgehog pathway inhibition, maybe move to surgery or maybe see or add consolidated adjuvant radiation therapy, which there's exciting evidence behind with the combination with hedgehog pathway inhibitors and have all fails or if appropriate for the patient, we have immunotherapy as an option, both from progression intolerance or contraindications for being on those other therapies that we can rely on. So a lot has changed in the last 10 years.
What factors guide your decision between a hedgehog pathway inhibitor and a PD-1 inhibitor?
Dr Patel: We generally think of hedgehog pathway inhibitors as the first-line treatment option. They are so effective. When we think about basal cell carcinoma, it's almost like a chronic disease, patients have it for decades, oftentimes years to decades. And so while we develop these oncologic studies to look at cure rates, complete response rate, partial response rate in a practical clinical setting, we just want to control the disease and hedgehog pathway inhibitors do that very well. It's the tolerability that's the issue. So the vast majority of approaches first-line approach is to start with hedgehog pathway inhibitors, unless there is some contraindication concern. Maybe somebody is very frail elderly and has low body weight, and we would be worried about decreased PO intake if they had dysgeusia, taste loss, a decrease intake of food. But the vast majority, I think are started on that. And then if patients can stay on it, we continue them on it.
But those chronic toxicities can have a significant impact quality of life. I mentioned, you can modify doses. We've learned how the difference between vismodegib and sonidegib, the pharmacokinetic differences, can be leveraged so that patients can potentially take breaks in the medication to minimize those side effects. And then if patients are not able to or they're having progression of disease, that usually is the decider for moving to an immunotherapy. It's generally reserved in the second-line setting. The immunotherapies are not only a very reasonable next step, but also because the effectiveness of that has been slightly lower, we may not reach for that in the first-line setting.
Now, one of the exciting new developments recently is that potentially there may be a higher signal with utilizing immunotherapies in our first-line setting. That means patients that are naive to hedgehog pathway inhibitors or potentially using combination immunotherapies such like as nivolumab with relatlimab or nivolumab and ipilimumab as shown by a recent study by the group out of John Hopkins, Evan Lipson's group that presented it at Mohs, which has really started to open our eyes and maybe we should be considering immunotherapy more earlier upfront, but this is an area where we need a little bit more evaluation and these decisions are best made in the multidisciplinary setting where we can collaborate with the dermatologists, the moh surgeons who are seeing these on the frontline, managing a lot of those hedgehog pathway inhibitors and toxicities along with the oncologists and thinking about immunotherapy.
Which patients are ideal candidates for immunotherapy, particularly among those who fail or cannot tolerate hedgehog inhibitors?
Dr Patel: The personalized treatment approach and figuring out the individualized treatment strategy is key to finding an ideal candidate. Understanding comorbidities, what the home life looks like, what is the support system? If there's a toxicity, can they tolerate which toxicity? An immune-mediated adverse event or dysgeusia, alopecia, muscle spasms, et cetera, et cetera. So having that holistic look, having the multidisciplinary evaluation is key. I would generally say the ideal candidates for immunotherapy are essentially patients where we are less worried about an adverse event that may be really detrimental or lead to a prolonged hospitalization. We worry about that in our older patients. And so thinking about treating somebody for longer periods of time with immunotherapy, that enters into our mindset because we do have another treatment option and hedgehog pathway inhibitors on the other hand, I would generally say we reach for those first and are thinking that the side effects are going to present, but we're going to adjust as depending on how much they present. But there are patients that have mobility issues where the muscle spasms may debilitate them, elderly patients, or as I mentioned earlier, that are very frail, have low body weights where any loss of weight, any decreased PO intake may be quite detrimental where the immunotherapy makes potentially a lot more sense where we know that those drugs are generally really well tolerated, but there can be unexpected side effects. So thinking about the patient holistically can help you pivot towards one way or the other and making that decision.